Dr Amal Mattu discusses his three favorite acute care articles of the past year. What are your top picks?
Professor and Vice Chair of Academic Affairs, Department of Emergency Medicine, University of Maryland School of Medicine, Baltimore, Maryland Once again, it is time for the annual review of my favorite articles of 2024.
The past year was chock-full of great literature relevant to emergency medicine , not only from the EM journals but also from many other specialty journals. As in past years, I am not choosing articles based on research methods and design. Rather, I am choosing articles that, in my opinion, have significant potential for immediately improving patient care. I believe these articles are practice-changers and, therefore, I recommend them as “must-reads.” They have high impact from a clinical and educational standpoint. I have chosen literature reviews based on the quality of evidence they summarize. They provide best-practice recommendations and give compelling arguments supporting a change in standard practice. My reviews will be brief, but I hope they will spark your interest to download and read the full manuscripts. Because of space limitations, I will limit this discussion to my three favorite articles of 2024.“My doctor told me to come to the emergency department to get checked out because my blood pressure was high. But I feel fine.” Every emergency physician has heard this, and it usually results in a feeling of frustration because of the time the patient has wasted, waiting to be told by you that everything is fine. Finally,Much of the text of this scientific statement from the American Heart Association endorses what is commonly taught in EM but not well known outside. First and foremost, the authors encourage clinicians to abandon the term “hypertensive urgency” and instead understand the dichotomy between patients having elevated blood pressure with acute end-organ damage vs those without acute end-organ damage. This latter group does not need urgent BP lowering and may actually do worse when attempts to rapidly lower the BP are made. Instead, physicians are urged to simply optimize oral BP regimens for this group.One other section of the article that I found enlightening was a discussion of how and why inaccurate BP measurements often occur. For example, the authorsindicating that when BPs are above 180/100 mm Hg, oscillometric devices may underestimate BP by as much as 50/30 mm Hg compared with BP readings from an arterial line.Given the importance of accurate BP acquisition in emergency department patients, it is critically important for healthcare providers to understand errors and limitations of routine BP measurements.is an excellent read. Furthermore, it is a valuable educational resource to share with your colleagues ─ especially those who routinely send patients with asymptomatic hypertension to the emergency department “to get checked out.”Ask most emergency physicians what their least favorite chief complaint is, and I’ll bet the vast majority will say “dizziness.” The challenge of “dizzy” is that it can mean so many things: vertigo, lightheadedness, near-, ataxia, nervousness, and so on. Asking patients to clarify whether they experienced any of the above options is often not helpful. My experience is that patients often change their answers to that question from one moment to the next, or they may select two or more possibilities. Even when patients explicitly say they experienced vertigo, or a sense of spinning, distinguishing whether the vertigo is central vs peripheral can be difficult. In recent years we have been taught to use specific maneuvers, such as the HINTS exam , but this is often difficult to perform accurately and can only be done while the patient is actively having vertigo and nystagmus. To correctly make this diagnosis is extremely important:called “Here’s My Take,” in which recognized experts in the field address controversial and challenging topics and provide evidence supporting their own best-practice recommendations. When it comes to the evaluation of dizziness, there is no greater expert in emergency medicine than Dr Jonathan Edlow. In this paper, he briefly addresses the HINTS exam as well an offshoot — the STANDING exam — and he provides some practical advice on how to evaluate and accurately diagnose the patient with dizziness when the clinician is uncomfortable with proper use of these maneuvers or when they cannot be performed. Edlow starts by reminding us that ED imaging of the acutely dizzy patient is rarely helpful in diagnosing peripheral vertigo vs. Even MRI with diffusion weighting can miss up to 20% of strokes in patients presenting within 48 hours of onset of isolated dizziness. Perhaps the most helpful feature in the history suggesting stroke is sudden onset of symptoms. Other symptoms that suggest stroke, rather than peripheral causes, include severe, neck pain, and an assortment of other neurologic symptoms that I often refer to as the “terrible D’s of dizziness”: dysarthria, dysphasia,, dysesthesias , and disequilibrium . Any focal weakness should also support stroke rather than a peripheral cause. On the other hand, dizziness suddenly occurring during sleep is suggestive of a peripheral cause. A detailed neurologic exam should be performed, especially focusing on testing the cranial nerves, including visual fields and hearing; and the cerebellar exam, including gait. Focal abnormalities of the neurologic exam strongly suggest a stroke. If nystagmus is present, its quality is critical to assess. Nystagmus due to a central cause is typically persistent and can be bidirectional or vertical. By contrast, nystagmus due to peripheral causes should be unidirectional, horizontal, with a latent onset, and that extinguishes with fixation . Edlow briefly describes other diagnostic algorithms besides HINTS and STANDING and he provides more details and pearls than the major ones I have provided in this limited space. The paper overall is an outstanding read from the leading educator on dizziness and is worth reading.The Society for Academic Emergency Medicine has been producing excellent clinical practice guidelines referred to as “GRACE” . The guidelines are practical, useful, and evidence-based, and I have enjoyed reading them. When this one was published, however, my initial reaction was one of skepticism: “What could I possibly need to know aboutthat I don’t already know?” In the inner-city ED in which I work, it is rare for a shift to go by when I don’t deal with both conditions. When I eventually read through the paper, however, I was surprised to find some very useful and, in fact, practice-changing information. I will focus on their recommendations regarding From the time I was in residency, I have always been a big fan of using high-dose benzodiazepines for alcohol withdrawal. Unfortunately, this practice is sometimes problematic. Part of the problem is that some patients require whopping doses of benzodiazepines, and oftentimes the nursing staff is just not comfortable administering these dosages; sometimes I’m not either. In those cases, we can add aas an alternative to benzodiazepines. Phenobarbital is a drug that some older practitioners may remember. When I was in residency training in the early 1990s, benzodiazepines had just recently replaced phenobarbital, and so I was not really familiar with its use. The authors of this paper encourage the use of phenobarbital in addition to benzodiazepines for tough cases of alcohol withdrawal that require admission. They cite literature suggesting that when phenobarbital is added to benzodiazepines for alcohol withdrawal vs use of benzodiazepines alone, there is a reduction in intubation and, a reduction in ICU admission rates and length of stay, an overall reduction in in-hospital length of stay, and a decreased need for physical restraints. The exact phenobarbital protocols were not discussed in detail, but they can easily be found on the internet. Here at University of Maryland Medical Center, we have created a protocol for patients with alcohol withdrawal utilizing phenobarbital and the results have been impressive. I have yet to see any concerning harmful effects of the protocol. The authors of this GRACE paper also address the use of anti-craving medication in patients who are being discharged with alcohol use disorder, as well as suggested therapies forhyperemesis syndrome. I will not address these recommendations here because of space limitations, but I do recommend that all emergency care practitioners peruse the recommendations.There you have it: my three favorite practice-changing, educational articles of 2024. I have only provided a brief review of the key take-home points, so I strongly recommend that all emergency care providers do a deep dive into each of these articles. I am confident you will find that the information these manuscripts provide will be enlightening and practice changing. Please be sure to include in the comments section your own pick for favorite or must-read articles of 2024. Best wishes to all for a safe and happy 2025! Amal Mattu, MD, is a professor, vice chair of education, and co-director of the emergency cardiology fellowship in the Department of Emergency Medicine at the University of Maryland School of Medicine in Baltimore. Follow Any views expressed above are the author's own and do not necessarily reflect the views of WebMD or Medscape.All material on this website is protected by copyright, Copyright © 1994-2025 by WebMD LLC. This website also contains material copyrighted by 3rd parties.
Otolaryngology ENT Specialty Head And Neck Surgery ENT Speciality Stroke Cerebrovascular Accident CVA Cerebrovascular Accident (CVA) Dizziness Vertigo Central Vertigo Benzodiazepines Vision Care And Maintenance Nystagmus Alcohol Use Cannabinoid Marijuana Clinical Guidelines Guidelines Ataxia Hypertensive Emergencies Maryland Residency Residents Cardiogenic Pulmonary Edema
United States Latest News, United States Headlines
Similar News:You can also read news stories similar to this one that we have collected from other news sources.
 AP Top 25: Big Ten, SEC each have four top 10 teams in women's pollThe Big Ten and the SEC both have seven teams ranked in The Associated Press Top 25 women's basketball poll released Monday.
AP Top 25: Big Ten, SEC each have four top 10 teams in women's pollThe Big Ten and the SEC both have seven teams ranked in The Associated Press Top 25 women's basketball poll released Monday.
Read more »
 Tennessee Remains Undefeated, Clinches Top Spot in AP Top 25Tennessee continues its dominance in college basketball, maintaining its No. 1 ranking in the AP Top 25 for the fifth consecutive week. Following two convincing victories, including a rout against SEC rival Arkansas, the Volunteers are the only undefeated team in men's Division I.
Tennessee Remains Undefeated, Clinches Top Spot in AP Top 25Tennessee continues its dominance in college basketball, maintaining its No. 1 ranking in the AP Top 25 for the fifth consecutive week. Following two convincing victories, including a rout against SEC rival Arkansas, the Volunteers are the only undefeated team in men's Division I.
Read more »
 AP Top 25: UCLA, South Carolina, Notre Dame remain on top in women's pollUCLA, South Carolina, Notre Dame kept the top three spots in the women's AP Top 25, while Minnesota entered for the first time since 2019.
AP Top 25: UCLA, South Carolina, Notre Dame remain on top in women's pollUCLA, South Carolina, Notre Dame kept the top three spots in the women's AP Top 25, while Minnesota entered for the first time since 2019.
Read more »
 Girls Wrestling Top 10 for Jan. 15: Top teams hold but major shakeup belowThe Top 10 girls wrestling teams in New Jersey ranked by dual meet strength
Girls Wrestling Top 10 for Jan. 15: Top teams hold but major shakeup belowThe Top 10 girls wrestling teams in New Jersey ranked by dual meet strength
Read more »
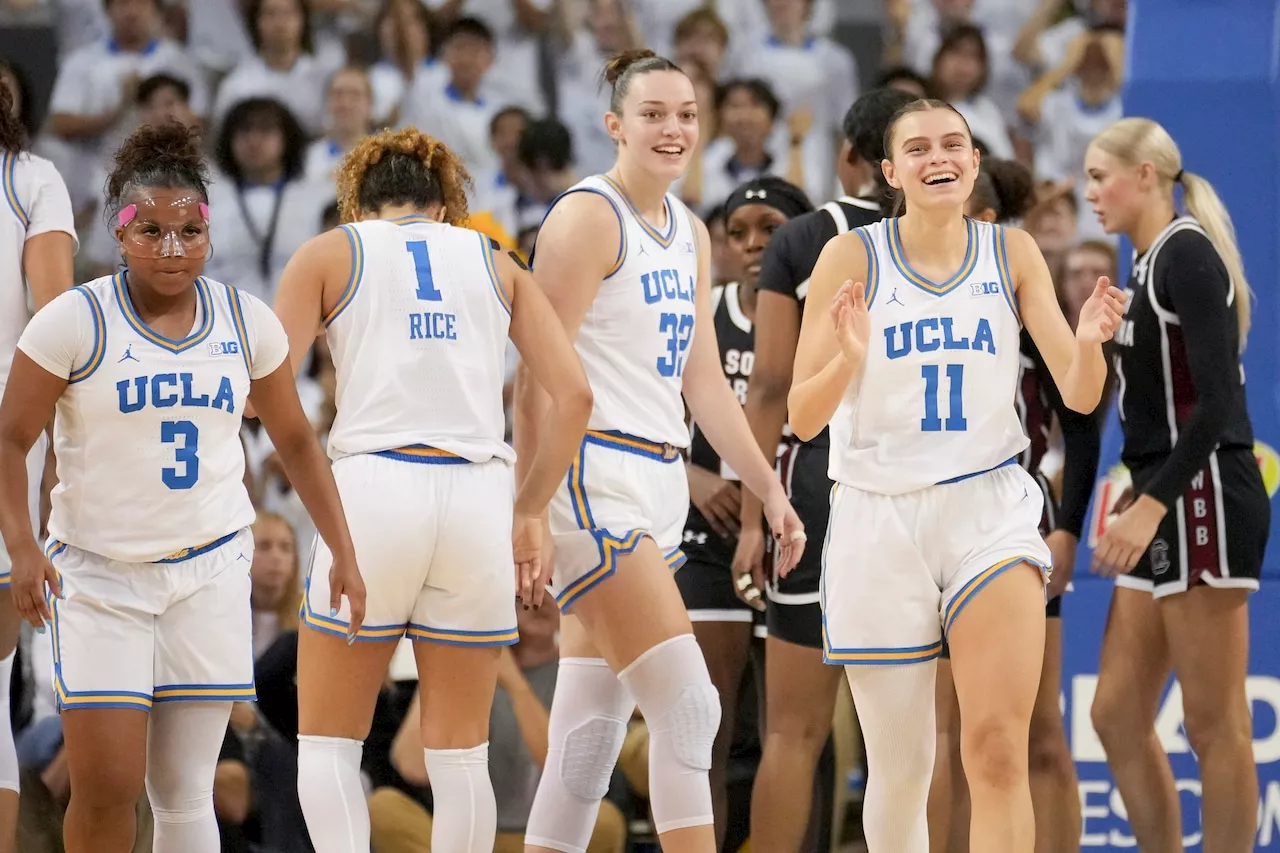 Top 25 Women's College Basketball Rankings: UCLA Remains No. 1, Minnesota Cracks Top 25UCLA holds onto the top spot in the AP Top 25 women's college basketball poll, while Minnesota makes its first appearance in the rankings since 2019 after a strong start to the season. The Golden Gophers have won 16 of their first 17 games. Other notable moves include LSU jumping to No. 5 and Oklahoma State re-entering the poll after defeating West Virginia.
Top 25 Women's College Basketball Rankings: UCLA Remains No. 1, Minnesota Cracks Top 25UCLA holds onto the top spot in the AP Top 25 women's college basketball poll, while Minnesota makes its first appearance in the rankings since 2019 after a strong start to the season. The Golden Gophers have won 16 of their first 17 games. Other notable moves include LSU jumping to No. 5 and Oklahoma State re-entering the poll after defeating West Virginia.
Read more »
 Vanderbilt Cracks Top 25, Texas Returns to Top FiveVanderbilt makes a triumphant return to the AP Top 25 after over a decade, securing the No. 23 spot. Texas climbs back into the top five, while Ohio State and Duke re-enter the top 10.
Vanderbilt Cracks Top 25, Texas Returns to Top FiveVanderbilt makes a triumphant return to the AP Top 25 after over a decade, securing the No. 23 spot. Texas climbs back into the top five, while Ohio State and Duke re-enter the top 10.
Read more »
