The Food and Drug Administration (FDA) has approved a bioengineered blood vessel developed by Humacyte to treat vascular trauma. This breakthrough technology addresses the critical need for blood vessel replacements in patients with injuries such as gunshot wounds, car accidents, and combat trauma. The engineered vessel, made from human-derived cells, mimics the natural structure and function of blood vessels, offering a safer and more durable alternative to synthetic grafts.
A new advance in tissue engineering could help. In December, the Food and Drug Administration approved a bioengineered blood vessel to treat vascular trauma . Made by North Carolina–based biotech company Humacyte , it’s designed to restore blood flow in patients with traumatic injuries, such as from gunshots, car accidents, industrial accidents, or combat.
“Some patients are so badly injured that they don't have any veins available,” says Laura Niklason, founder and CEO of Humacyte. Even when a patient has a usable one, a vein often isn’t a good replacement for an artery. “Your veins are very thin. They're weak little structures, and your arteries are very strong,” she says. Niklason first became interested in the idea of growing spare blood vessels in the 1990s, when she was training to be a physician at Massachusetts General Hospital. She remembers observing a patient undergoing a heart bypass, which involves using a healthy vessel to reroute blood flow around a blocked coronary artery. The surgeon opened up both of the patient’s legs, arms, and finally, the stomach, in search of a suitable blood vessel to use. “It was just really barbaric,” Niklason says. She figured there had to be a better way. She started with growing blood vessels in the lab from just a few cells collected from pig arteries. When she transplanted them into the animal, they worked like the real thing. After those early experiments, it was a long road to an FDA-approved product for humans. Niklason and her team spent more than a decade isolating blood vessel cells from human organ and tissue donors. They tested cells from more than 700 donors and found that those from five of those donors were the most efficient at growing and expanding in the lab. Niklason says Humacyte now has enough cells banked from these five donors to make between 500,000 and a million engineered blood vessels. The company currently makes the vessels in batches of 200, using custom-designed degradable polymer scaffolds that are 42 centimeters long and 6 millimeters thick. The scaffolds are placed in individual bags and seeded with millions of the donor cells. The bags then go into a school-bus-sized incubator to soak in a nutrient bath for two months. While the tissue grows, it secretes collagen and other proteins that provide structural support. Eventually, the polymer scaffold dissolves and the cells are washed away with a special solution. What’s left is “de-cellularized” flexible tissue in the shape of a blood vessel. Because it doesn’t contain living human cells, it won’t cause rejection when implanted into a patient. “People have been trying to come up with a tubular material like this one for a long time,” says Anton Sidawy, president-elect of the American College of Surgeons and a vascular surgeon at the George Washington University Medical Center, who isn’t involved with Humacyte. Currently, synthetic alternatives made of Teflon or a type of polyester called Dacron are sometimes used when a patient doesn’t have an available blood vessel. But they’re not ideal. “Every time you put a foreign body in the human body, the chance of infection goes up. Bacteria love to sit on the foreign body and cause an infection,” Sidawy says. The safety and effectiveness of the engineered vessel was tested in 51 civilian patients and 16 military patients with traumatic injuries, and the results were compared with previous studies of people who received synthetic versions. At 30 days after implantation, nearly 92 percent of the vessels remained open and functioning, compared with 79 percent for synthetic grafts. About 4.5 percent of patients required amputation, much lower than the 24 percent in tests of synthetic grafts. In addition, less than 1 percent of the bioengineered vessels became infected compared with more than 8 percent for the synthetic options. The results were published in the journal JAMA Surgery in November. “This actually becomes part of the patient's body,” says Michael Curi, chief of vascular surgery at Rutgers New Jersey Medical School, who coauthored the paper. “The body grows its own cells into this vessel wall, and it mimics a natural vessel.” While the December approval means Humacyte’s vessel can only be used in trauma patients, the company is pursuing other uses for its technology. It has tested the bioengineered vessel in patients on kidney dialysis, which requires connecting an artery or vein to a dialysis machine, as well as in individuals with peripheral artery disease, when arteries in the legs or arms become blocked. In monkeys, a smaller version of the engineered blood vessel has also shown promise in treating heart bypass. “It’s truly a remarkable scientific achievement,” Curi says. “And in my opinion, it is the future of medicine.”
Tissue Engineering Bioengineered Blood Vessel Vascular Trauma FDA Approval Humacyte
United States Latest News, United States Headlines
Similar News:You can also read news stories similar to this one that we have collected from other news sources.
 New Study Identifies How Blood Vessel Dysfunction Can Worsen Chronic DiseaseA research team has uncovered new mechanisms in blood vessel formation, revealing how blood vessel dysfunction can worsen chronic diseases. The studies highlight the unique characteristics of blood vessels in the lungs and their role in pulmonary hypertension. Additionally, the research explores the role of microglia in regulating blood flow and maintaining brain blood vessels, which could have implications for cognitive health. 3D microvessels have also been created to observe red blood cell transit, shedding light on how these cells deliver oxygen and nutrients.
New Study Identifies How Blood Vessel Dysfunction Can Worsen Chronic DiseaseA research team has uncovered new mechanisms in blood vessel formation, revealing how blood vessel dysfunction can worsen chronic diseases. The studies highlight the unique characteristics of blood vessels in the lungs and their role in pulmonary hypertension. Additionally, the research explores the role of microglia in regulating blood flow and maintaining brain blood vessels, which could have implications for cognitive health. 3D microvessels have also been created to observe red blood cell transit, shedding light on how these cells deliver oxygen and nutrients.
Read more »
 AI Spotting Eye Blood Vessel 'Fingerprints' Linked to Stroke RiskA new study used AI to identify 29 unique blood vessel patterns in the retina that are significantly associated with an increased risk of stroke. Researchers believe this technique could help identify potential stroke risks earlier, leading to preventative measures.
AI Spotting Eye Blood Vessel 'Fingerprints' Linked to Stroke RiskA new study used AI to identify 29 unique blood vessel patterns in the retina that are significantly associated with an increased risk of stroke. Researchers believe this technique could help identify potential stroke risks earlier, leading to preventative measures.
Read more »
Marvel Rivals Season 1: Eternal Night Falls Introduces Blood Soldier and Blood Kariudo SkinsNew skins for Winter Soldier and Psylocke arrive in Marvel Rivals, coinciding with the Vampire-themed Season 1.
Read more »
 How Outlander: Blood of My Blood Could Make Outlander Season 8 Even BetterStarz's Outlander spinoff, Blood of My Blood, set to premiere before the final season of Outlander, could significantly elevate the stakes and intrigue surrounding the show's conclusion. By exploring the love stories of Jamie and Claire's parents, the spinoff could shed light on the origins of their romance, and perhaps even hint at the fate of Claire's stillborn daughter, Faith.
How Outlander: Blood of My Blood Could Make Outlander Season 8 Even BetterStarz's Outlander spinoff, Blood of My Blood, set to premiere before the final season of Outlander, could significantly elevate the stakes and intrigue surrounding the show's conclusion. By exploring the love stories of Jamie and Claire's parents, the spinoff could shed light on the origins of their romance, and perhaps even hint at the fate of Claire's stillborn daughter, Faith.
Read more »
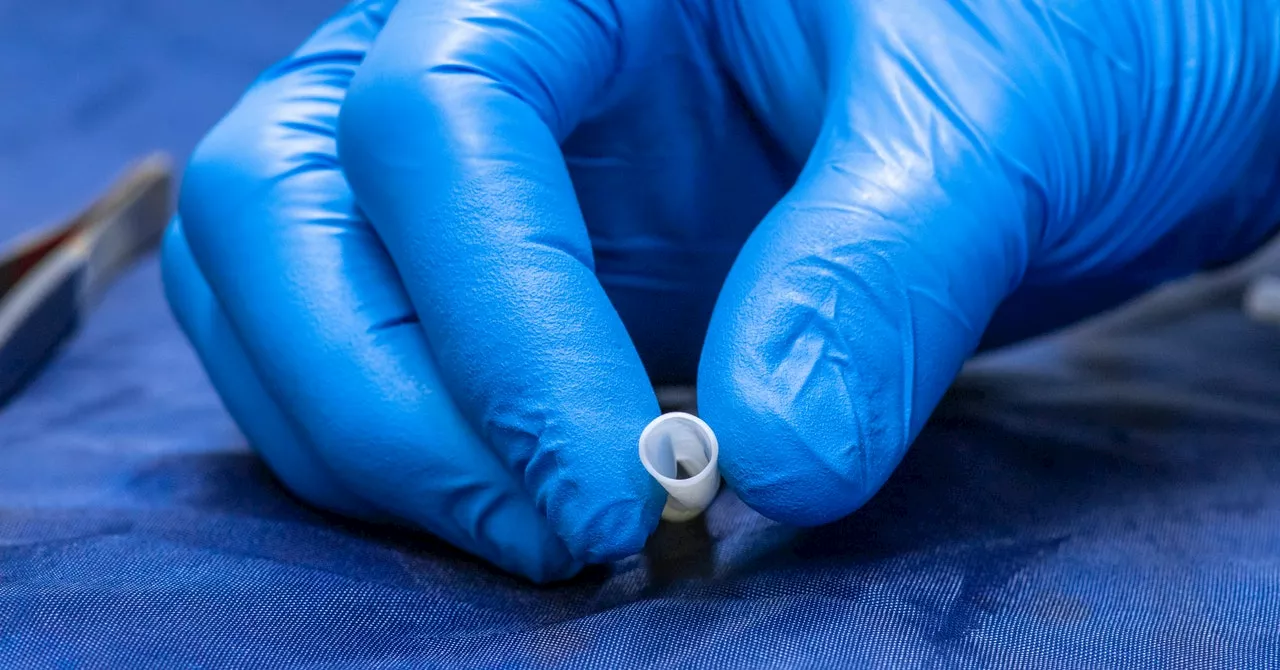 This Blood Vessel Was Grown in a Lab With Real Human CellsThe FDA recently approved a bioengineered blood vessel, which becomes part of a patient’s body over time. It’s designed to help treat victims of traumatic injuries.
This Blood Vessel Was Grown in a Lab With Real Human CellsThe FDA recently approved a bioengineered blood vessel, which becomes part of a patient’s body over time. It’s designed to help treat victims of traumatic injuries.
Read more »
 Alaska Blood Bank Urges Residents to Donate During National Blood Donor MonthThe Blood Bank of Alaska faces a constant need for blood donations to meet the demands of Alaskan hospitals. The article highlights the shortage of donors in the state and emphasizes the importance of individual contributions to ensure a stable blood supply for all Alaskans.
Alaska Blood Bank Urges Residents to Donate During National Blood Donor MonthThe Blood Bank of Alaska faces a constant need for blood donations to meet the demands of Alaskan hospitals. The article highlights the shortage of donors in the state and emphasizes the importance of individual contributions to ensure a stable blood supply for all Alaskans.
Read more »
